Gum Disease and Breast Cancer: What the Latest Research Reveals About Oral Health Risks
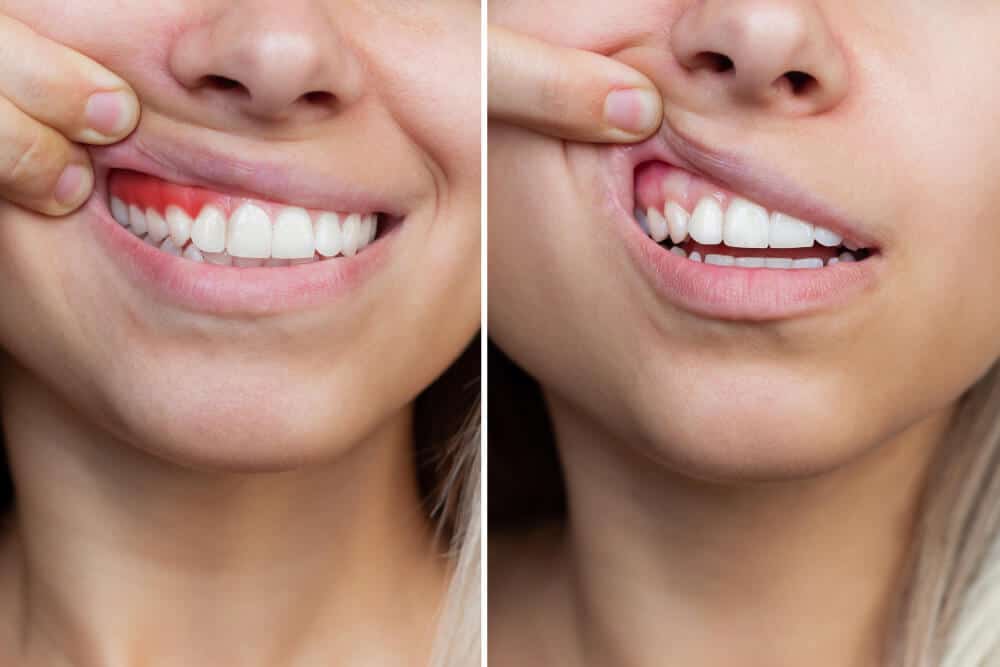
Most people know that gum disease causes bleeding gums, bad breath, and — if ignored long enough — tooth loss. But what if the consequences extended far beyond your mouth?
New research from Johns Hopkins Medicine has uncovered a direct link between a common gum disease bacterium and breast cancer. It is the kind of finding that changes how we think about oral health, and it is exactly why regular dental care matters more than most people realise.
If you live in Cheltenham or the surrounding area, this is worth reading.
What the Research Found
Fusobacterium nucleatum is a bacterium most people have never heard of. Yet, it lives in the mouths of those with gum disease and, according to new research, can travel well beyond the mouth — settling in breast tissue where it may cause harm.
The study, published in Cell Communication and Signaling, found that this bacterium can enter the bloodstream, travel through the body, and settle in breast tissue, where it triggers inflammation and early cellular changes associated with cancer development.
This is not the first time Fusobacterium nucleatum has appeared in cancer research. It was previously connected to colorectal cancer. But this study is among the first to draw a clear line between the bacterium and breast cancer, adding weight to what several smaller studies had already begun to suggest — that periodontal disease and breast cancer risk may be connected.
For patients who may have been putting off a dental check-up, this research is a timely reminder that oral health and general health are not separate conversations.
How the Bacterium Affects the Body
Understanding what this bacterium actually does inside the body helps explain why researchers are taking the findings seriously.
When Fusobacterium nucleatum enters breast tissue, it does not sit passively. In laboratory experiments, introducing the bacterium into breast ducts caused abnormal cellular changes — some cells multiplied excessively, others changed type entirely. These changes were accompanied by DNA damage, ongoing inflammation, and increased cell division.
Using animal models designed to replicate human breast cancer, the team observed that the bacterium contributed to faster tumour progression and a greater likelihood of cancer cells spreading to the lungs.
The bacterium also interferes with the body’s ability to repair damaged DNA. It activates an error-prone repair process that quickly reconnects broken DNA strands but does so imprecisely, introducing mutations along the way. Even short-term exposure to the bacterium raised levels of a protein linked to increased cancer cell movement, invasion, stem-like behaviour, and resistance to chemotherapy.
These are not minor effects. The research suggests this bacterium actively disrupts how cells function — and the longer gum disease goes untreated, the longer it remains in the body.
Why Some People Face a Higher Risk
One of the most significant findings in the study involves people who carry BRCA1 gene mutations — a genetic variation already known to raise the risk of breast cancer significantly.
Researchers found that breast cells with BRCA1 mutations were far more vulnerable to Fusobacterium nucleatum than other cells. These cells carry elevated levels of a surface sugar that makes it easier for the bacterium to attach and enter.
As a result, BRCA1-mutant cells absorbed more of the bacterium, held onto it across multiple cell generations, and experienced more sustained DNA damage and cancer-promoting effects.
For anyone who carries a BRCA1 mutation and is already managing elevated cancer risk, this finding adds oral health to the list of modifiable factors worth addressing proactively. It does not replace other medical guidance, but it does suggest that healthy gums may play a role in a broader prevention picture.
What Is Gum Disease and How Do You Know If You Have It?
Gum (periodontal) disease is a condition in which bacterial buildup causes ongoing damage to the gums, the connective tissue, and the bone that support teeth. It develops when plaque builds up along and below the gum line, causing the gums to become inflamed. Left untreated, it progresses from mild inflammation (gingivitis) to a more serious infection that damages the bone supporting the teeth.
It is also far more common than most people realise. Many Australians live with some degree of gum disease without knowing it, because the early stages are often painless.
Signs to watch for include:
- Bleeding gums during brushing or flossing
- Red, swollen, or tender gums
- Gums that look like they are receding or sitting lower than usual around the teeth
- Persistent bad breath that does not resolve with brushing
- Teeth that feel loose or have shifted position
- Sensitivity along the gum line
If any of these sound familiar, it is worth booking a check-up. Gum disease at any stage is treatable, and the earlier it is caught, the more straightforward the treatment.
The Broader Picture: Oral Health and Systemic Health
The Johns Hopkins research adds to a growing body of evidence linking the health of the mouth to that of the rest of the body. This connection, also called the oral-systemic link, is an area of increasing focus in dental and medical research.
Fusobacterium nucleatum is not the only oral bacterium that has been linked to conditions elsewhere in the body. Research has also linked gum disease to cardiovascular disease, with studies showing that bacteria from the mouth can infiltrate the heart and contribute to the buildup of scar tissue.
Separate research has found associations between periodontal disease and elevated blood pressure, cognitive decline, and complications in diabetes management.
The mouth is not isolated from the rest of the body. The gums are highly vascular tissue — meaning they have a rich blood supply.
Chronic gum inflammation creates an environment where bacteria can pass through the gum tissue and gain access to the bloodstream. From there, they can travel to organs and tissues throughout the body.
This is why dentists talk about oral health as part of overall health, not as a separate concern. A healthy mouth reduces bacterial load in the body, lowers systemic inflammation, and removes a potential source of ongoing tissue harm elsewhere.
Practical Steps to Support Healthy Gums
The encouraging part of this research is that gum disease is largely preventable — and, once it has developed, treatable. There are practical steps every person can take to reduce their risk.
- Brush thoroughly, twice a day. Use a soft-bristled toothbrush and fluoride toothpaste. Spend at least 2 minutes brushing, making sure to clean along the gum line, not just the tooth surfaces.
- Floss or use interdental brushes daily. Plaque builds up between the teeth and below the gum line, where a toothbrush cannot reach. Flossing removes this buildup before it hardens into tartar, which can trigger gum inflammation.
- Attend regular dental check-ups and professional scale and clean. Even with excellent home care, tartar accumulates over time and can only be removed professionally. Routine appointments allow your Cheltenham dentist to detect changes in your gum health at an early stage, when they are easier to manage.
- Do not ignore bleeding gums. Bleeding when you brush or floss is one of the earliest signs of gum disease. It is not normal and should not be dismissed. If your gums bleed regularly, mention it at your next appointment.
- Avoid smoking. Smoking weakens the mouth’s immune response, allowing gum disease to develop and progress more aggressively — and because it can mask typical warning signs, the condition often goes undetected for longer.
- Manage conditions that affect gum health. Diabetes, for example, increases susceptibility to gum infections. If you have a condition that affects immune function, talk to your dentist about a more proactive monitoring schedule.
When to See a Dentist
If it has been more than six months since your last check-up, now is a good time to book. You do not need to wait until something is painful — in fact, waiting for pain is one of the most common reasons gum disease progresses further than it needs to.
A dental check-up will include an assessment of your gum health. During an assessment, your dentist will check the space between your gums and teeth, known as periodontal pockets, which provide a reliable measure of gum health and help guide any recommended care.
The Johns Hopkins research is still developing. However, the evidence points in the same direction: oral health is connected to whole-body health in ways that are still being uncovered, and maintaining healthy gums is one of the most practical things you can do for your long-term wellbeing.
Frequently Asked Questions About Gum Disease and Oral Health
Does gum disease directly cause breast cancer?
The research does not establish that gum disease directly causes breast cancer. What the Johns Hopkins study found is that a bacterium associated with gum disease may contribute to DNA damage and tumour growth when it reaches breast tissue. More clinical studies are needed before a direct causal relationship can be confirmed. What the evidence does support is that untreated gum disease is worth taking seriously for overall health reasons.
Should I be concerned if I have gum disease and a BRCA1 mutation?
The research found that cells carrying BRCA1 mutations were more susceptible to the effects of Fusobacterium nucleatum. If you carry a BRCA1 mutation, it is worth discussing your oral health as part of your broader health management with both your dentist and your GP or specialist. Keeping gum disease under control is a practical and achievable step alongside any other preventive measures you are already taking.
How do I know if I have gum disease?
Many people have gum disease in its early stages without any pain, which is why regular dental check-ups are so important. If you have noticed any changes in your gums — such as bleeding, swelling, or persistent bad breath — mention them at your next visit. Your dentist can assess your gum health thoroughly and identify any concerns early.
Can gum disease be reversed?
When caught early, gingivitis can often be brought under control through a thorough professional cleaning combined with consistent home care. More advanced gum disease, called periodontitis, cannot be fully reversed but can be effectively managed and controlled with the right treatment. The key is addressing it early.
How often should I have my gums checked?
For most people, a check-up every six months is sufficient to monitor gum health and catch any early changes. Patients with a history of gum disease or other contributing risk factors may require more frequent monitoring. Your dentist will advise on a recall schedule suited to your circumstances.
Is gum disease common in Australia?
Yes. Gum disease is one of the most prevalent oral health conditions in Australia, and a significant number of adults have some degree of it — often without realising it. The painless nature of early-stage gum disease means it frequently goes undetected until it has progressed. Regular professional check-ups remain the most reliable way to stay on top of it.
Book Your Gum Health Check in Cheltenham
At Dentist On Warrigal Cheltenham, we take gum health seriously — because the research increasingly shows that we should. Whether you are due for a routine check-up or you have noticed changes in your gums, we are here to help you stay on top of your oral health.
Call us on (03) 9583 5506 or book online at a time that suits you. Visit us at Suite C, 151 Centre Dandenong Road in Cheltenham — conveniently located for patients coming from Highett, Mentone, Moorabbin, Bentleigh, and across the surrounding area.

